Advancements in Ceramic Materials for Orthopedic Implants
The field of orthopedic surgery has been revolutionized by the development of advanced biomaterials designed to replace or support damaged bones and joints. Among these, ceramic materials have emerged as a critical class of implants due to their exceptional biocompatibility, wear resistance, and mechanical properties. This article explores the latest advancements in ceramic materials used for orthopedic implants, focusing on their evolution, current applications, and future potential.
1. Key Properties of Ceramic Biomaterials
Ceramics are inorganic, non-metallic materials that offer a unique combination of properties ideal for orthopedic applications. Their success in implantology stems from several inherent characteristics:
1.1 Biocompatibility and Bioinertness
High-purity ceramics like alumina (Al2O3) and zirconia (ZrO2) are bioinert, meaning they do not elicit significant immune responses or toxic reactions when implanted in the body. This promotes stable, long-term integration with host tissues.
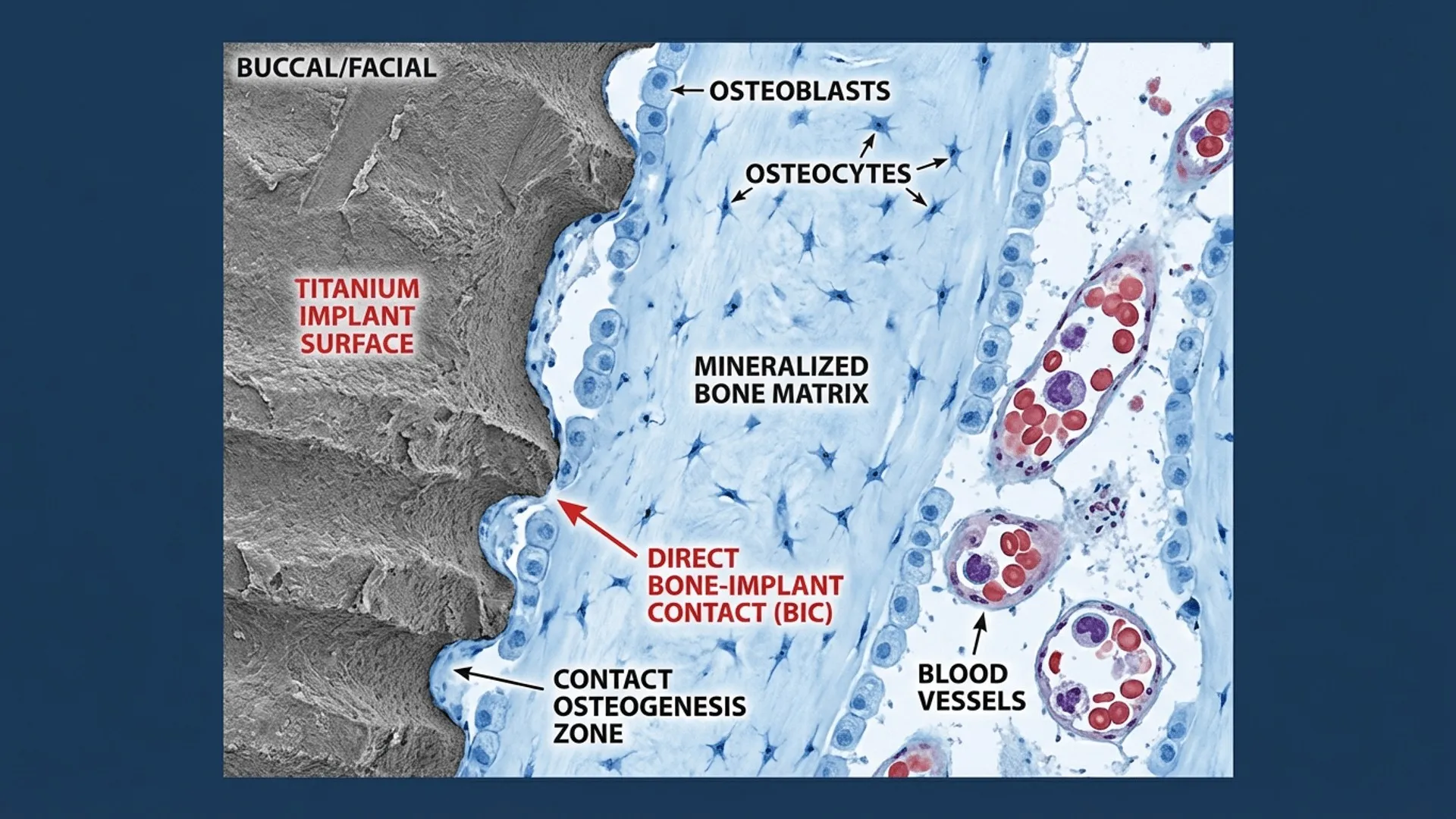
1.2 Wear Resistance and Low Friction
Ceramics exhibit extreme hardness and low coefficients of friction. In joint replacements, particularly hip and knee bearings, this results in minimal particulate wear debris, reducing osteolysis (bone resorption) and implant loosening.
1.3 Mechanical Strength and Fatigue Resistance
Advanced ceramics possess high compressive strength, making them suitable for load-bearing applications. Modern processing techniques have significantly improved their fracture toughness, addressing historical concerns about brittleness.
2. Evolution and Types of Orthopedic Ceramics
The development of ceramics for orthopedics has progressed through generations, from first-generation bioinert ceramics to third-generation bioactive and resorbable materials.
2.1 First-Generation: Bioinert Ceramics
Alumina and Zirconia are the workhorses of bioinert ceramics.
- Alumina: Used since the 1970s, it offers excellent corrosion resistance and hardness. Modern high-purity, fine-grained alumina has superior strength.
- Zirconia: Introduced to overcome alumina's brittleness, zirconia has higher fracture toughness due to a phenomenon called "transformation toughening."

2.2 Second-Generation: Bioactive Ceramics
These materials, such as Hydroxyapatite (HA) and certain glass-ceramics (e.g., Bioglass®), form a direct chemical bond with living bone. They are often used as coatings on metallic implants to enhance osseointegration.
2.3 Third-Generation: Resorbable and Composite Ceramics
The latest advancements focus on ceramics that actively participate in bone remodeling. Tricalcium phosphate (TCP) is a resorbable material that is gradually replaced by new bone. Furthermore, ceramic-polymer composites and ceramic-ceramic composites (like zirconia-toughened alumina) are being developed to tailor mechanical and biological properties.
3. Clinical Applications and Performance
Ceramic materials are now standard in several orthopedic applications.
| Material | Key Properties | Primary Applications | Advantages |
|---|---|---|---|
| Alumina (Al2O3) | High hardness, bioinert, excellent wear resistance | Femoral heads, acetabular liners (Hip), knee components | Long-term durability, low wear rates |
| Zirconia (ZrO2) | High fracture toughness, good flexural strength | Femoral heads, dental implants | Reduced risk of fracture vs. early alumina |
| Hydroxyapatite (HA) | Bioactive, osteoconductive, similar to bone mineral | Coatings on hip/knee stems, bone graft substitutes | Promotes rapid bone ingrowth and fixation |
| Zirconia-Toughened Alumina (ZTA) | Combined high wear resistance and toughness | Modern hip replacement bearings | Superior mechanical reliability |
3.1 Total Hip Arthroplasty (THA)
Ceramic-on-ceramic (CoC) and ceramic-on-polyethylene (CoP) bearings are widely used. CoC bearings demonstrate the lowest in-vivo wear rates, making them ideal for younger, more active patients.
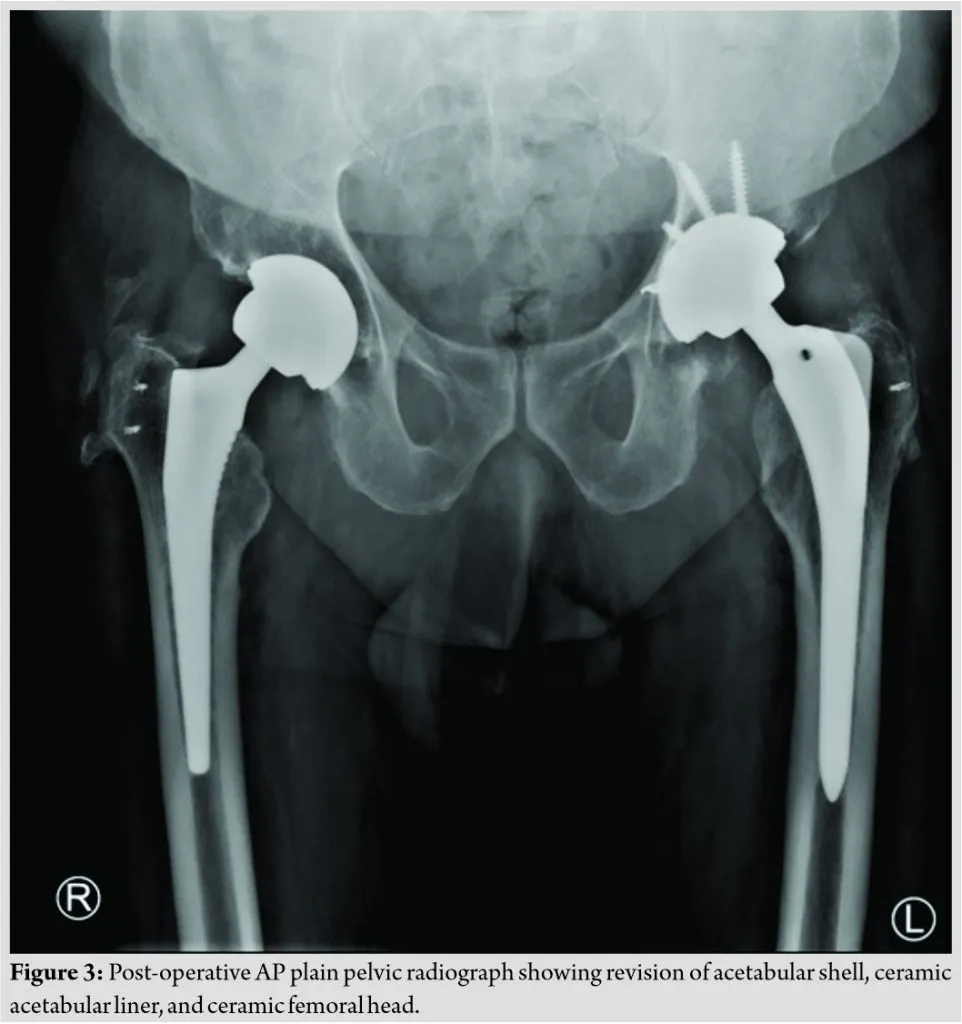
3.2 Total Knee Arthroplasty (TKA)
While less prevalent than in hips, ceramic femoral components are gaining traction due to their scratch resistance and potential for longer polyethylene insert longevity.
4. Current Challenges and Research Frontiers
Despite successes, challenges remain, driving ongoing research.
4.1 Addressing Brittle Fracture Risk
While rare, implant fracture is a concern. Research is focused on novel manufacturing (e.g., hot isostatic pressing), nanostructuring, and advanced composite designs to enhance reliability.
4.2 Enhancing Osseointegration
Surface modification techniques, such as creating porous ceramic structures or adding bioactive ion coatings (strontium, silicon), are being developed to accelerate and strengthen bone bonding.
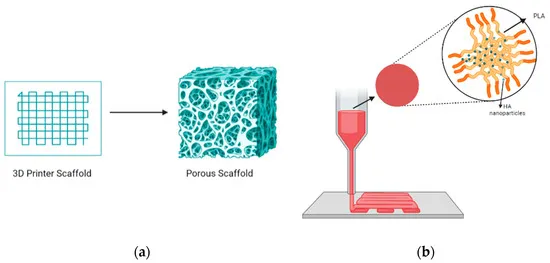
4.3 3D Printing and Patient-Specific Implants
Additive manufacturing (3D printing) of ceramics allows for the creation of complex, patient-specific geometries and controlled porous architectures that mimic natural bone.
5. Future Directions and Conclusion
The future of orthopedic ceramics lies in smart, multifunctional materials. This includes ceramics with drug-eluting capabilities for infection prevention, materials with tailored degradation rates for bone regeneration, and the integration of digital technologies for optimized implant design.
In conclusion, ceramic materials have solidified their role as indispensable components in modern orthopedic implantology. From bioinert bearings that last decades to bioactive scaffolds that stimulate healing, continuous innovation in material science, processing, and design promises to further improve patient outcomes, implant longevity, and quality of life for millions worldwide.

